Dogs entering their senior years still have significant time ahead. How that time goes depends largely on what happens in the first year after the transition.
The threshold of "senior" in dogs is not a fixed age. A Great Dane is elderly at seven. A Beagle at seven is roughly middle-aged. A Chihuahua may not qualify as senior until nine or ten. Body size is the primary determinant because larger dogs age faster at the cellular level, driven in part by higher IGF-1 (insulin-like growth factor) levels that accelerate metabolic processes.
For most medium-to-large breeds, the veterinary consensus places the senior threshold at seven years. This article uses that benchmark, while acknowledging that giant breeds should apply its advice two years earlier and small breeds may wait a year or two longer.
What follows is the body-system-by-system account of what actually changes, which changes are normal aging and which signal disease, and what evidence-based management looks like at each stage.
Musculoskeletal: The Joints and Muscles
Osteoarthritis is the most prevalent condition in dogs over seven. The Banfield Pet Hospital State of Pet Health report consistently shows it as a top-five diagnosis in senior dogs, with prevalence rising steeply after age eight. The joint changes start years before any visible signs appear.
What normal aging looks like: a dog that sleeps more, plays with slightly less intensity, and takes slightly longer to warm up after rest. These are physiological slowing. What disease looks like: a dog that hesitates before climbing stairs it managed easily six months ago, that holds one leg differently, that flinches when touched in the lumbar region or over a hip, or that gets up from sleep significantly more stiffly than before.
The distinction matters because normal aging does not respond to NSAID therapy. Arthritis does. A dog whose reduced activity is actually pain-driven will often show marked improvement within 72 hours of appropriate pain management. If your vet prescribes a two-week NSAID trial and the dog's behavior changes visibly, that was not aging. That was treatable disease you can now continue to manage.
Weight management is the most powerful intervention. Every kilogram of excess body weight adds roughly three to four kilograms of force through each joint during a normal walking stride. A dog already losing cartilage cannot afford that added stress. A 2002 study in the Journal of the American Veterinary Medical Association showed that lean body-conditioned Labrador Retrievers had a median lifespan 1.8 years longer than their heavier littermates and developed arthritic signs three years later.
Physical therapy and controlled low-impact exercise, swimming in particular, maintains joint range of motion and preserves periarticular muscle mass without the impact loading of running on hard surfaces. Certified canine rehabilitation practitioners (CCRP) provide structured programs for senior dogs that are worth the investment for dogs with moderate-to-advanced arthritis.
Cognitive Changes: Normal Aging Brain vs. CDS
Canine Cognitive Dysfunction Syndrome (CDS), often described as the dog equivalent of Alzheimer's disease, affects an estimated 28% of dogs aged 11 to 12 years and 68% of dogs aged 15 to 16. The condition involves accumulation of beta-amyloid plaques in the brain and progressive neuronal loss.
The classic CDS checklist, often summarized as DISHA, covers: Disorientation (getting lost in familiar spaces, staring at walls), Interactions changing (less interest in people or family, or conversely, increased clinginess), Sleep-wake cycle reversal (active at night, sleeping during the day), House soiling (losing previously reliable housetraining), and Activity level changes (decreased interest in play, exploration, or food).
"I see dogs that have been 'getting old' for two years that actually have moderate-to-advanced cognitive dysfunction. The owners thought it was normal. It's not. It's a disease with treatments that can slow it."
Dr. Gary Landsberg, veterinary behaviorist, North Toronto Animal ClinicNormal cognitive aging in dogs looks different: slightly slower learning of new tasks, somewhat reduced responsiveness to commands the dog has known for years, modestly decreased activity. These are gradual and mild. CDS is progressive and functional: a dog that cannot find its way to its food bowl in a house it has lived in for ten years does not have normal aging. It has a disease.
Current treatments include selegiline (Anipryl), approved for CDS in dogs, which increases dopamine and reduces free radical damage in neural tissue. Dietary interventions with omega-3 fatty acids, medium-chain triglycerides, and antioxidants (available in senior prescription diets like Hill's b/d) show modest evidence of slowing progression. Environmental enrichment, novel toys, food puzzles, and regular low-intensity training, maintains cognitive engagement and is part of every management protocol.
Organ Systems: What Changes and When
Kidneys: Chronic kidney disease (CKD) affects approximately 10% of dogs, with prevalence rising significantly after age seven. The kidneys lose functional nephrons over time through a combination of aging, prior infections, toxin exposures, and genetic predisposition. Dogs compensate by concentrating urine with the remaining nephrons. The first sign owners often notice is increased water intake and urination, as the kidneys lose concentrating ability. By the time BUN and creatinine rise outside normal ranges, 75% of nephron function may already be lost. Annual urine specific gravity measurement and a senior chemistry panel are the only way to catch this early.
Heart: Mitral valve disease (MVD) is the most common cardiac condition in senior dogs, particularly small breeds. A grade 1 or 2 murmur found at a senior wellness exam can be managed with medication (pimobendan, ACE inhibitors) that has been shown in the EPIC trial to significantly delay the onset of congestive heart failure. Large breed dogs are more susceptible to dilated cardiomyopathy (DCM), particularly Dobermans, Boxers, and Irish Wolfhounds. Biannual echocardiography is recommended for high-risk breeds starting at age five or six.
Liver: Hepatic function declines with age, but the liver has enormous functional reserve. Significant liver disease typically does not produce symptoms until 70 to 80% of function is lost. Annual liver enzyme panels catch elevations before clinical signs develop. Dogs with elevated ALP or ALT at a wellness visit warrant follow-up assessment even if they appear completely healthy.
Endocrine: Hypothyroidism and Cushing's disease (hyperadrenocorticism) both become more common after seven. Hypothyroid dogs gain weight, lose coat quality, become lethargic, and may develop skin infections. It is often attributed to aging. Cushing's dogs drink excessively, lose muscle mass, develop a pot-bellied appearance, and may have thin skin with hair loss. Both are treatable with appropriate medication, and dogs typically show significant quality-of-life improvement within weeks of starting treatment.
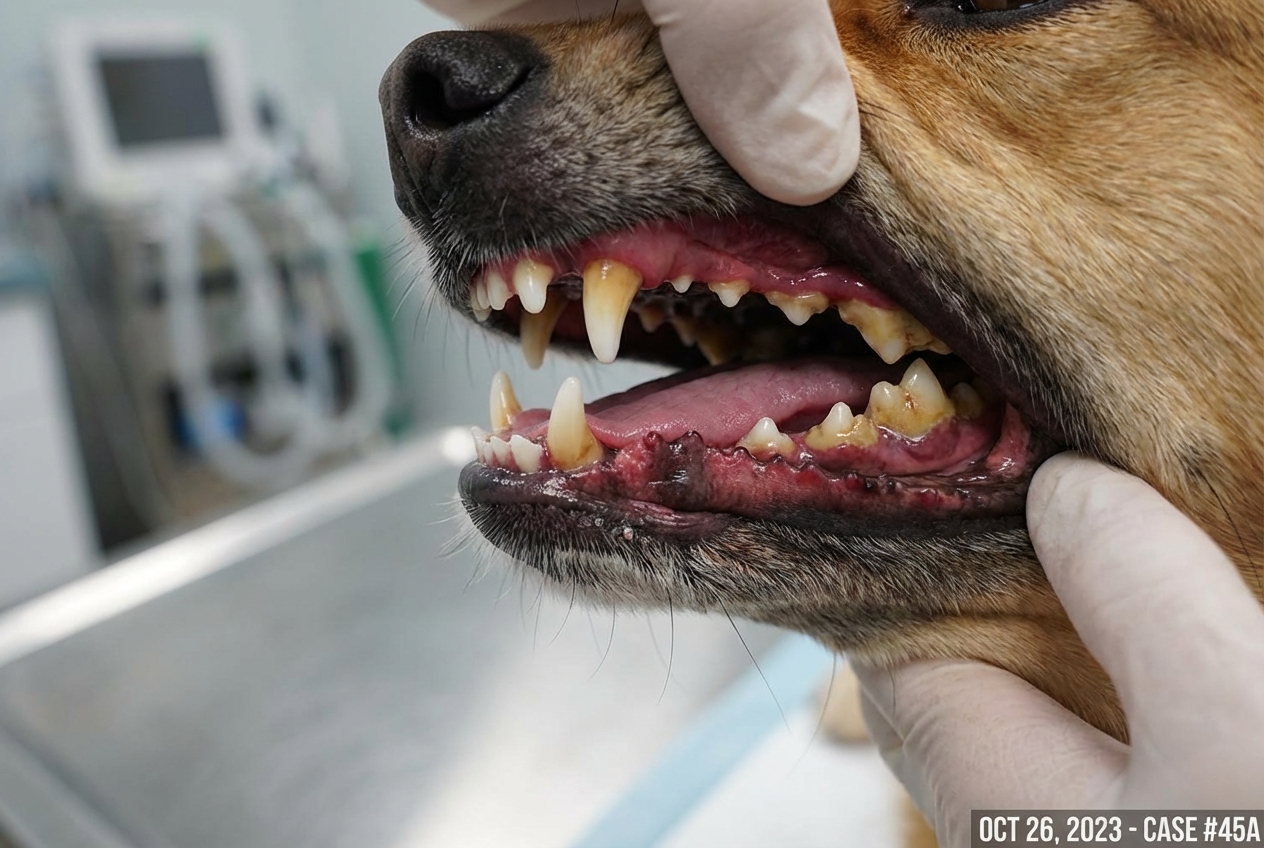
Senior dogs face dental disease on top of everything else
See where your dog stands with our free 60-second assessment designed specifically for older dogs.
Take the QuizDental Health in Senior Dogs: The Compounding Problem
Senior dogs typically carry years of accumulated periodontal disease. A 10-year-old dog with no dental care history may have Grade 3 or 4 periodontal disease affecting most of its teeth. This creates a specific management challenge: dental cleanings require anesthesia, and senior dogs, particularly those with heart or kidney disease, carry higher anesthetic risk than healthy adults.
The answer is not to avoid dental care. The answer is pre-anesthetic bloodwork, cardiac evaluation where indicated, and careful anesthetic protocol selection. Veterinary anesthesiologists and internal medicine specialists routinely manage cleanings in dogs with controlled heart murmurs, early kidney disease, and other senior conditions. The risk of continued periodontal disease, including the systemic bacteremia and organ damage discussed in our dental disease article, typically outweighs the carefully managed anesthetic risk.
Between professional cleanings, home dental care becomes even more important in senior dogs. Dogs that have never accepted toothbrushing are very unlikely to start at age nine. This is one area where enzymatic dental products that work through a dog's own licking behavior become particularly relevant. An at-home dental approach that does not require brushing or restraint is worth knowing about, especially for owners managing senior dogs with established dental disease and limited tolerance for handling.
The Twice-Yearly Exam After Seven
The standard recommendation from both the AAHA and the AVMA is twice-yearly wellness visits for dogs over seven. This is not a revenue-generation strategy. It reflects the rate at which age-related conditions progress and the value of six-month surveillance versus twelve-month surveillance in animals whose biological year moves faster than a human's.
A senior wellness panel typically adds SDMA (symmetric dimethylarginine), a more sensitive early marker of kidney function decline than BUN or creatinine, to the standard chemistry panel. It may also include a urine protein-to-creatinine ratio, a complete blood count, and thyroid hormone levels. The full panel runs $200 to $400 depending on the practice. Run annually at minimum, and twice yearly in dogs over ten or those with known organ system disease.
What You Can Actually Do
The practical checklist for a dog crossing into senior years is not complicated, but it requires consistency. Book a baseline senior wellness visit with a full chemistry panel, urinalysis, CBC, and blood pressure measurement. Discuss the findings with your vet and establish a monitoring calendar. Assess body condition score and make dietary adjustments if the dog carries excess weight. Evaluate the current diet for senior-appropriate protein and phosphorus levels, and discuss whether a senior or prescription diet is appropriate based on any organ system findings.
Watch the water bowl. Increased water intake is one of the most reliable early signs of kidney disease, diabetes, Cushing's, or pyometra in intact females. Get a rough baseline on how much your dog drinks in a 24-hour period. A useful benchmark: more than 100 mL per kilogram per day warrants a veterinary discussion.
Watch the floor. A dog that slips on hardwood more than it used to is losing muscular control in its hindquarters. This may be arthritis. It may be degenerative myelopathy, a progressive spinal condition common in German Shepherds, Corgis, and Boxers. It may be a spinal lesion. None of these is "just getting old" in the sense of being untreatable.
The goal is not to stop your dog from aging. The goal is to distinguish what can be treated from what cannot, address what can, and give your dog the best possible function in the years it has. That starts with paying attention to the specific, concrete changes rather than absorbing them as background noise under the heading of "getting old."
For more on the signs that distinguish aging from disease, read our guide to 7 warning signs your dog is hiding pain. For a full picture of what a senior wellness exam covers, see what actually happens during a dog wellness exam.